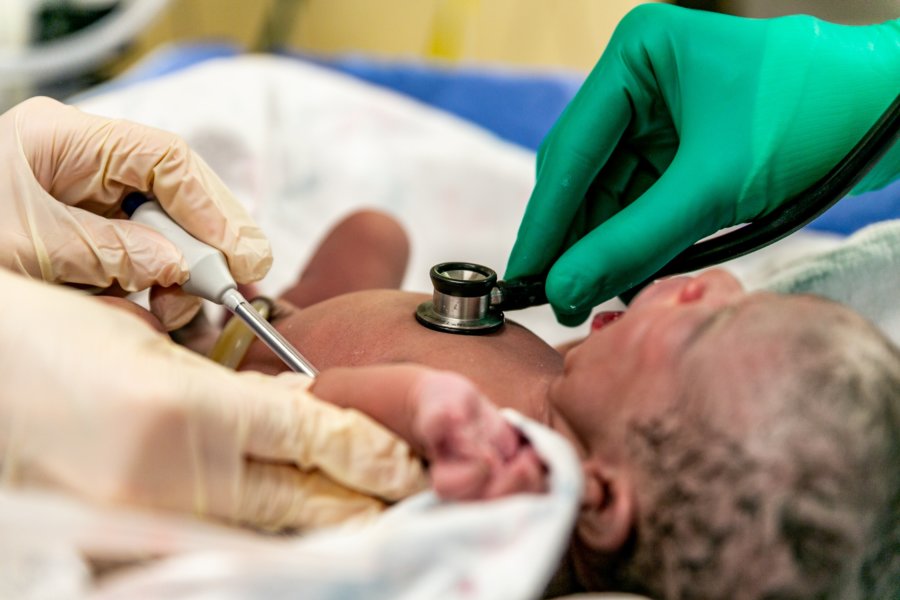
Infants rely on their parents or caretakers to provide them with adequate nutrition needed for healthful physical and mental growth. Some babies aren’t able to receive nutrition via a bottle or a feeding tube due to developmental problems, disease or extreme prematurity. Parenteral nutrition may be necessary to help these infants get the calories and nutrients they need to thrive.
What is Total Parenteral Nutrition?
Parenteral nutrition was first given to babies more than 50 years ago. It has saved thousands of infants’ lives who are unable to take in enough calories and nutrients. The term parenteral refers to bypassing the digestive tract. Total parenteral nutrition means that all of the infants nutrition is delivered in this manner.
Nutrition in the form of carbohydrates, protein, fat, minerals, vitamins and electrolytes are given intravenously in total parenteral nutrition. This can be done by using an injection, but it typically requires that an IV be placed in the navel, hand, scalp or foot.
Emergency versus Ongoing Total Parenteral Nutrition
Preterm infants are often given parenteral nutrition immediately following their birth. This can give these babies the boost of nutrients they need to adjust to life outside of the womb. Total parenteral nutrition may continue to be given as the baby learns to use a bottle or breastfeed. When total parenteral nutrition is going to occur for a short time, medical professionals use smaller veins in a central location on the infant’s body to deliver the nutrients.
In some cases, an infant will need to receive total parenteral nutrition on an ongoing basis. This may be due to kidney or digestive tract problems. If ongoing parenteral nutrition is needed then a central line may be placed in the infant. This allows a larger amount of nutrients to quickly flow to the baby.
Success of Total Parenteral Nutrition in Newborns
Though there are some risks of continuing total parenteral nutrition in newborns, most do extremely well. Several studies have been done that compare the effect of milk feedings versus total parenteral nutrition in preterm infants with very low birthweights. Studies showed that these infants fared extremely well with total parenteral nutrition. The infants receiving total parenteral nurtiion were able to take in larger amounts of protein and carbohydrates versus the infants who were fed a milk diet.