As technology has aided in advanced medical care over the last few decades, neonatology treatments and care options have improved and grown in number. Maternal mortality prevention is the goal of neonatology, and these trends are helping caregivers achieve their goals.
Here are a few prevailing neonatology trends to keep an eye on in 2020.
More Resources for Practicing Neonatologists
There are more available than ever for practicing neonatologists, primarily because of the growing need for more highly capable practitioners. The increasing number of mothers who are addicted to drugs or alcohol, increasingly poor nutrition, diabetes and high blood pressure are some driving factors of this trend. Neonatologists and medical professionals with similar disciplines can connect with the Section on Neonatal-Perinatal Medicine (SONPM) website, which is an affiliate of the American Academy of Pediatrics.
Preventing Neonatal Sepsis
Neonatal sepsis is another condition that affects millions of children every year. This is a bacterial bloodstream infection (BSI) that is potentially life-threatening to babies, especially those of low birth-weight. This can happen quite unexpectedly and for many reasons, including pneumonia, meningitis and gastroenteritis. This makes the detection of neonatal sepsis before it fully takes hold of the child imperative. Treatments can be applied speedily to rid the bloodstream of the infection when it’s detected early.
Improving Communication with Parents
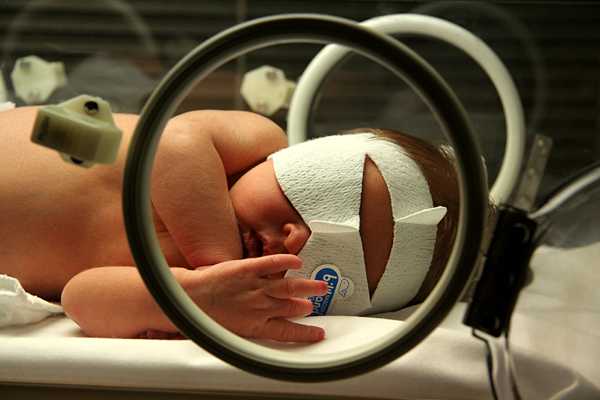
When your newborn child is in the intensive care unit (ICU), it can be the most trying experience of your life. To reduce the stress and anxiety that can come from not knowing, neonatologists are trying to be more transparent and open to communicating with the parents. In cases of premature infants, this can mean encouraging skin-to-skin contact between the parents and the baby. Research has even shown the babies’ vital signs tend to suddenly improve when they are being held by their parents. The relief the parents feel to know their child is in good care is an added benefit.
With the help of specialized supplements for newborn babies, malnutrition is no longer a problem. However, optimizing the use of breastmilk is a tradition that most neonatologists are trained to believe in. Breastfeeding is encouraged, but when this can’t happen, donor milk is promoted as an option before other methods for nutrition aid are considered.